Melanoma
Megan Brennard, BS and Kesha Buster, MD
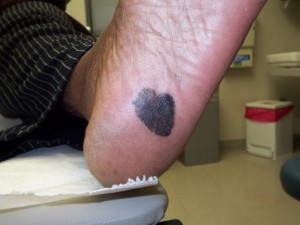 Skin cancer is the most common type of cancer in the United States. Melanoma is the third most common type of skin cancer and the most deadly.1 Darker skinned people all have relatively low risk of melanoma compared to whites.1 Though uncommon in people of color, blacks and Hispanics are more often diagnosed with more advanced melanomas, and they often have higher mortality than whites.1-3 It has been observed that fairer-skinned persons have a higher rate of melanoma than darker-skinned persons–even within the same ethnic group. Accordingly, whites have an overall greater incidence than Hispanics, who have a higher incidence than blacks and Asians.1 Though it can appear on any skin surface, the common locations for melanoma on people of color are on non-sun-exposed skin including the bottoms of the feet, the palms, finger- and toenails, and inside of the mouth.1,4
Skin cancer is the most common type of cancer in the United States. Melanoma is the third most common type of skin cancer and the most deadly.1 Darker skinned people all have relatively low risk of melanoma compared to whites.1 Though uncommon in people of color, blacks and Hispanics are more often diagnosed with more advanced melanomas, and they often have higher mortality than whites.1-3 It has been observed that fairer-skinned persons have a higher rate of melanoma than darker-skinned persons–even within the same ethnic group. Accordingly, whites have an overall greater incidence than Hispanics, who have a higher incidence than blacks and Asians.1 Though it can appear on any skin surface, the common locations for melanoma on people of color are on non-sun-exposed skin including the bottoms of the feet, the palms, finger- and toenails, and inside of the mouth.1,4
What is the cause of melanoma?
In whites, increased exposure to ultraviolet radiation (UVR), including sunlight and tanning beds, is a significant risk factor for melanoma. UVR may also play a role in melanoma development in people of color, as blacks and Hispanics living closer to the equator (getting greater UVR exposure) have higher melanoma incidence, but this link is less-well established.5 In whites, more than 90% of melanomas are on sun-exposed skin.1 In contrast, nearly 75% of melanomas in people of color are on the palms, soles, mucosal sites (mouth, genitals) and under nails.1 Additional reported melanoma risk factors in people of color include radiation therapy, preexisting pigmented lesions, albinism, burn scars, and depressed immune system.1
How do I know if I have melanoma?
Any suspicious, changing, or new mole or freckle anywhere on your skin should be evaluated by your dermatologist. However, because many melanomas on dark skin are found on poorly visible areas, you should do a monthly self-skin examination. An easy way to remember the signs of melanoma is by the ABCDEs,6 a memory-aid for how to evaluate pigmented lesions:
A ‐ Asymmetry. Pigmented lesions should look the same on both sides when folded in half.
B ‐ Border irregularity. The borders should be smooth and regular–usually round or oval in shape.
C ‐ Color variation. The lack of uniform and even color.
D ‐ Diameter. Size of greater than 6mm or about the size of a pencil eraser.
E ‐ Evolving. Any change (including size, shape, color) in an existing mole or skin lesion
Also, because of the higher incidence of melanoma in a fingernail or toenail in people of color, the “alphabet of nail melanoma” is a useful guide for self and physician examinations7:
A – Age range 20-90 years
African-American, Native American, or Asian
B – Band of Brown or Black pigment in nail OR
Breadth of >3mm OR
Border that is irregular/blurred
C – Change in size or growth rate of nail band OR
lack of Change in irregular nail despite treatment
D – Digit involved (nail melanoma is most common in the thumb>big toe>index finger)
Pigmented band on a single Digit is more suspicious
Dominant hand involvement is more common
E – Extension of brown or black pigment to the side or base of the nail
F – Family or personal history of melanoma or irregular moles
In addition, any pigmented lesion that looks different than the majority of one’s moles and freckles (i.e., an ‘ugly duckling’) should be evaluated.
What are the best treatments for melanoma?
Any lesion suspicious for melanoma should be biopsied or completely excised (removed). Once melanoma is diagnosed, if the lesion was not completely removed initially, a second procedure will be done to remove all of the cancer with margins of normal skin. Depending on the depth, your dermatologist may send you to a cancer surgeon for removal and analysis of lymph nodes to determine if the melanoma has spread. Metastatic (distantly spread) melanoma is treated with various combinations of chemotherapy, radiation, interferons, and medications through clinical studies.
Melanoma may be less common in people of color, but when found early, there is a very high cure rate. Diagnosing melanoma in later stages is associated with a poorer prognosis. As such, patients should be proactive in examining all skin surfaces. Any concerning lesion should be brought to the attention of your dermatologist or other physician.
Download Spanish translation.
Descarga traducción en español.
Additional Resources
The Skin Cancer Foundation
American Cancer Society
Melanoma Foundation
References
- Gloster HM, Neal K. Skin cancer in skin of color. J Am Acad Dermatol, 2006;55:741-60.
- Byrd KM, Wilson DC, Hoyler SS, Peck GL. Advanced presentation of melanoma in African Americans. J Am Acad Dermatol 2004;50:21-4.
- Weinstock MA. Nonmelanoma skin cancer mortality in the United States. Arch Dermatol 1993;129:1286-90.
- Nestle O, Helmut K. Melanoma. In: Bolognia, JL, Jorrizo JL, Rapini R, editors. Dermatology 2nd Ed. New York: Mosby; 2003. p.1780-1816.
- Hu S, Fangchao M, Collado-Mesa F, Kirser RS. UV radiation, latitude, and melanoma in US Hispanics and blacks. Arch Dermatol 2004;140:819-24.
- Abbasi NR, Shaw HM, Rigel DS, Friedman RJ, McCarthy WH, Osman I, Kopf AW, Polsky D. Early diagnosis of cutaneous melanoma: Revisiting the ABCD Criteria. JAMA 2004;292:2771-6.
- Levit EK, Kagen MH, Scher RK, Grossman M, Altman E. The ABC rule for clinical detection of subungal melanoma. J Am Acad Dermatol 2000;42 Part 1:269-74.

Cutis Journal
Read published peer-reviewed articles written your by Skin of Color Society members

Did You Know
Skin of color patients comprise the majority in California, New Mexico and Texas…and soon will be the majority in Arizona, Nevada, Georgia, New York and Florida.
By 2042, more than 50% of the US population will have skin of color.




