Nonmelanoma Skin Cancer (NMSC)
Jennifer Turnham, BS and Kesha Buster, MD
What are Nonmelanoma Skin Cancers?
Skin cancer is the most common malignancy in the United States and represents approximately 35‐45% of all cancers in Caucasians, 4‐5% in Hispanics, and 1‐4% in Asians , Asian Indians and African‐Americans.1‐3 Although skin cancer occurs less frequently in dark‐skinned people, it is often associated with greater morbidity and mortality compared to light‐skinned individuals.3‐4 Therefore, it is important for people of all races to be aware of the risks of both melanoma‐‐the most deadly type of skin cancer‐‐and other more common types which are collectively termed non‐melanoma skin cancer (NMSC). Squamous cell carcinoma (SCC) and basal cell carcinoma (BCC) are the two most common forms of NMSC.
SCC accounts for approximately 20% of all skin cancers and about 75% of all deaths due to skin cancer, excluding melanoma.5,6 It is the most common skin cancer in African-Americans and Asian Indians and the second most common skin cancer in Hispanics, Asians (Chinese and Japanese) and Caucasians.3 BCC is the most common skin cancer in Hispanics, Chinese and Japanese Asians, and Caucasians.3 Though BCC can be locally destructive, it rarely metastasizes (spreads).
What is the cause of NMSC?
NMSC has many causes. Ultraviolet (UV) radiation from sunlight, scarring processes, chronic injury, and depressed immune system (e.g., after organ transplantation) all contribute to the development of NMSC. UV radiation is the primary cause of both SCC and BCC in Caucasians, Hispanics, and Asians.3 However, the most important predisposing factors for the development of SCC in African-Americans are chronic scarring, trauma, and inflammation (e.g., burns, non-healing leg ulcers, skin lupus), not sun-exposure.7 The main risk factor for BCC in all races is UV radiation.8 Darker skin color does provide a protective effect, however, as BCC is more common in lighter skinned- versus darker-skinned African-Americans.7
How do I know if I have NMSC?
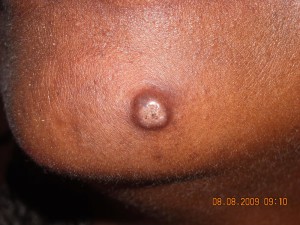
NMSC can look many different ways. Both SCC and BCC may be without symptoms, or grow slowly over time with associated pain or spontaneous bleeding. In dark-skinned individuals, SCC tends to occur in skin that is unexposed such as the legs, anus, and genitals whereas in lighter-skinned people, sun-exposed skin is the most common site.8 BCCs most often occur in the head and neck regions in all races. These most commonly present as painless, shiny, solitary bumps. Like SCCs, these may have a tendency to bleed easily. In people of color, more than 50% of BCCs have pigment (dark color), as opposed to only 5% in Caucasians.3,9 If any new lesion is painful, bleeding, growing, changing, or is otherwise concerning to you, it should be evaluated by your dermatologist.
What are treatments for NMSC?
There are many treatment options for NMSC. The most appropriate form of treatment depends on the size of the tumor, location, and type of skin cancer. Your dermatologist should help determine which treatment is right for you.
Excisional surgery remains the most common method for treating NMSC. It is effective in treating small, low-risk tumors.
Mohs micrographic surgery (MMS) is especially useful in treating large tumors and those on certain areas of the face. This method allows surgeons to ensure that all malignant tumor extensions are removed by mapping the edges of the excised tumor and analyzing it under a microscope.10
Electrodesiccation and curettage (ED&C) is another widely accepted method of treating low-risk NMSC. During this procedure, an electrical current is used to destroy tissue that is subsequently scraped off using a slim sharp instrument known as a curette. This method usually leaves a round scar.
Cryosurgery is another technique used in the treatment of NMSC. This technique uses liquid nitrogen to freeze the tumor tissue. After freezing, the area typically blisters before healing in three to four weeks.
Nonsurgical options
In addition to surgical techniques, topical immunomodulators, such as imiquimod, have gained recent FDA approval for treatment of thin NMSC. These treat the skin cancer by boosting the local immune system to kill the tumor. Another option is photodynamic therapy (PDT), which is a combination of a topical photosensitizing cream and a specialized light. Additionally, 5-fluorouracil cream (a chemotherapeutic agent) can be used to treat NMSC. All topical options have the benefit of treating NMSC with less risk for scarring. However, unlike MMS, excision or ED&C, complete cure cannot be ascertained and topical agents cannot be used on large or deep tumors. Overall the cure rates are lower and recurrences more common than with surgical treatments.11 Lastly, radiation is used on large or high-risk tumors that cannot be completely treated with surgery.
Download Spanish translation.
Descarga traducción en español.
Additional Resources
The Skin Cancer Foundation
American Cancer Society
References
1. Ridky TW. Non-melanoma skin cancer. Journal of the American Academy of Dermatology 2007;57:484-501.
2. Halder RM, Bridgeman‐Shah S. Skin cancer in African Americans. Cancer 1995;75(2
Suppl):667‐673.
3. Gloster HM, Neal K. Skin cancer in skin of color. Journal of the American Academy of
Dermatology 2006;55:741‐760.
4. Weinstock MA. Nonmelanoma skin cancer mortality in the United States. Arch Dermatol
1993;129:1286‐90.
5. Byrd‐Miles K, Toombs EL, Peck GL. Skin cancer in individuals of African, Asian, Latin‐
American, and American‐Indian descent: Differences in incidence, clinical presentation,
and survival compared to Caucasians. Journal of Drugs in Dermatology 2007;6:10‐16.
6. Kwa RE, Campana K, Moy RL. Biology of cutaneous squamous cell carcinoma. Am Acad
Dermatol 1992;26:1‐26.
7. Halder RM, Bang KM. Skin cancer in African Americans in the United States.
Dermatologic Clinics 1988;6:397‐405.
8. McCall CO, Chen SC. Squamous cell carcinoma of the legs in African Americans. Journal
of American Academy of Dermatology 2002;47:524‐529.
9. Bigler C, Feldman J, Hall E, Padilla RS. Pigmented basal cell carcinoma in Hispanics.
Journal of the American Academy of Dermatology 1996;34:751‐752.
10. Otley CC and Roenigk RK. Mohs Surgery. In: Bolognia, JL, Jorrizo JL, Rapini R, editors.
Dermatology, 2nd Ed. New York: Mosby; 2003. p. 2331‐2340.
11. Rigel DS, Cockerell CJ, Carucci J, Wharton J. Actinic Keratosis, Basal Cell Carcinoma, and
Squamous Cell Carcinoma In: Bolognia, JL, Jorrizo JL, Rapini R, editors. Dermatology 2nd
Ed. New York: Mosby; 2003. p. 1677‐1696.

Cutis Journal
Read published peer-reviewed articles written your by Skin of Color Society members

Did You Know
Skin of color patients comprise the majority in California, New Mexico and Texas…and soon will be the majority in Arizona, Nevada, Georgia, New York and Florida.
By 2042, more than 50% of the US population will have skin of color.




