Mycosis Fungoides
Zainab Mohammodu MHS, Brittany Shaw, Ali Al-Haseni, MD, Prince Adotama, MD
Reviewed and edited by: Neelam Vashi, MD and Stavonnie Patterson, MD
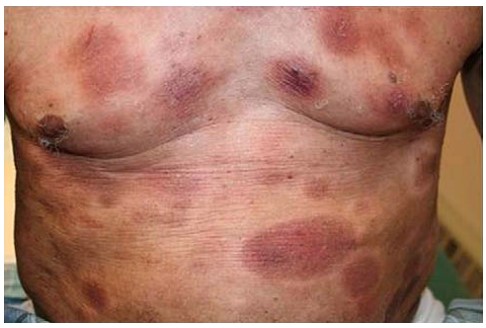
Figure 1: Adult Jamaican patient diagnosed with mycosis fungoides.1
What is Mycosis Fungoides?
Mycosis Fungoides (MF) is a rare slow growing cancer that originates from T-cell lymphocytes residing in the skin. T-cells, found in the blood, lymph nodes and the skin, are specialized types of white blood cells in the immune system that can undergo cancerous transformation. Mycosis Fungoides is the most common type of cutaneous T-cell lymphoma.2 Recent studies have shown MF to be more common in patients with skin of color. Black populations, in particular, have shown an increase in morbidity and mortality with Mycosis Fungoides.3,4 Increased mortality rates may be attributed to the failure of recognizing early signs of the disease in darker skin tones. 5
What is the cause of Mycosis Fungoides?
Although the incidence of MF has increased in recent years, MF is still regarded as a rare disease with just over 5000 new cases being reported annually.6 MF is not hereditary nor contagious and the exact cause has yet to be determined. However, there is promising research that MF could be related to genetic abnormalities caused by viruses, or exposure to cancer causing substances throughout one’s lifetime. Further research is still needed to determine the cause for MF.
How do I know if I have Mycosis Fungoides?
MF can be seen with a variety of manifestations in skin of color and can often be misdiagnosed for other skin conditions that mimic its characteristics. 3 A skin biopsy of the area is very important for early diagnosis of MF. 7 Classic presentations of MF show itchy red patches (flat rash) and plaques (raised rash) affecting the skin. The patches can often have a wrinkled appearance. Patients with MF can experience a range of disease expressions from having just one singular patch to having multiple plaques, usually found in sun-protected areas like the breasts, groin, buttocks or inner surfaces of the arms and legs.8 In more advanced cases, MF can also be associated with large lumps (tumors) that sometimes ulcerate through the skin. Lymph nodes and internal organs could also become involved in more advanced disease, but are usually spared in the majority of patients. Hypopigmented MF is subtype of MF, that is more common in people of color; and it presents with patches that are lighter in color (hypopigmented). These spots are typically asymptomatic (do not cause symptoms), but can become itchy in some patients. This type of MF almost never spreads to organs other than the skin, and has an excellent prognosis (outcome), and response to phototherapy (light treatment).
What are the best treatments for Mycosis Fungoides?
Medications used for MF fall into two categories: skin-directed treatment and systemic treatment.
Skin-directed treatment involves the application of ointments or gels directly to the affected areas of the skin. Topical therapies include topical steroids, nitrogen mustard, topical bexarotene, and imiquimod cream. Phototherapy, either with narrowband ultraviolet-B (UVB) or ultraviolet-A (UVA) light, is considered the first line therapy for extensive skin involvement in the early stages of classic MF or for all patients with hypopigmented MF. For thicker, more persistent plaques resistant to phototherapy, Total Skin Electron Beam (TSEB) radiation therapy is another option. Skin-directed treatment is often the first line of treatment in MF as most lymphoma cells are only found on the surface of the skin. 1
Systemic treatment involves the intake of medications by mouth or through an infusion. Systemic treatment is usually reserved for patients with more advanced disease. This is typically given for large lumps (tumors) on the skin, widespread thick rash covering > 10% of body area, erythrodermic MF (redness covering > 90% of the body), or for internal organ involvement. Treatments are varied and include oral bexarotene, methotrexate, extracorporeal photopheresis, romidepsin, pralatrexate, doxorubicin, and many other chemotherapeutic and systemic regimens.9
Some treatments are given on a daily basis, while others are given every few weeks or months. The therapy usually continues for many months to years. However, it can be stopped once the affected skin gets better and the patient no longer has symptoms. If one therapy is unsuccessful, alternative options are usually available and can be initiated.10 Once the disease has appropriately responded, it is important to remember that sometimes maintenance treatment is needed to ensure the disease stays in remission. Patients are highly encouraged to follow up with their dermatologists, even when their disease is clear, to detect any recurrence and to initiate treatment as early as possible.
References
- Hinds, G. A., & Heald, P. (2009). Cutaneous T-cell lymphoma in skin of color. Journal of the American Academy of Dermatology, 60(3), 359-375. doi:10.1016/j.jaad.2008.10.031
- Larocca, C., & Kupper, T. (2019). Mycosis Fungoides and Sézary Syndrome: An Update. Hematology/oncology clinics of North America, 33(1), 103–120. https://doi.org/10.1016/j.hoc.2018.09.001
- Criscione, V. D., & Weinstock, M. A. (2007). Incidence of Cutaneous T-Cell Lymphoma in the United States, 1973-2002. Archives of Dermatology, 143(7). doi:10.1001/archderm.143.7.854
- Weinstock, M. A., & Gardstein, B. (1999). Twenty-year trends in the reported incidence of mycosis fungoides and associated mortality. American Journal of Public Health, 89(8), 1240-1244. doi:10.2105/ajph.89.8.1240
- Sun, G., Berthelot, C., Li, Y., Glass, D. A., 2nd, George, D., Pandya, A., Kurzrock, R., & Duvic, M. (2009). Poor prognosis in non-Caucasian patients with early-onset mycosis fungoides. Journal of the American Academy of Dermatology, 60(2), 231–235. https://doi.org/10.1016/j.jaad.2008.09.063
- Amorim, G. M., Niemeyer-Corbellini, J. P., Quintella, D. C., Cuzzi, T., & Ramos-E-Silva, M. (2018). Clinical and epidemiological profile of patients with early stage mycosis fungoides. Anais brasileiros de dermatologia, 93(4), 546–552. https://doi.org/10.1590/abd1806-4841.20187106
- Pimpinelli, N., Olsen, E. A., Santucci, M., Vonderheid, E., Haeffner, A. C., Stevens, S., Burg, G., Cerroni, L., Dreno, B., Glusac, E., Guitart, J., Heald, P. W., Kempf, W., Knobler, R., Lessin, S., Sander, C., Smoller, B. S., Telang, G., Whittaker, S., Iwatsuki, K., … International Society for Cutaneous Lymphoma (2005). Defining early mycosis fungoides. Journal of the American Academy of Dermatology, 53(6), 1053–1063. https://doi.org/10.1016/j.jaad.2005.08.057
- Aun, J., Patel, H., Patel, K., Cashman, J., & Bailey, E. (2018, July 01). Perplexing Rash: Challenges to Diagnosis and Management of Mycosis Fungoides. Retrieved December 08, 2020, from https://jaoa.org/article.aspx?articleid=2686419
- Zic, J. A., Ai, W., Akilov, O. E., Carter, J. B., Duvic, M., Foss, F., . . . Geskin, L. J. (2020). United States Cutaneous Lymphoma Consortium recommendations for treatment of cutaneous lymphomas during the COVID-19 pandemic. Journal of the American Academy of Dermatology, 83(2), 703-704. doi:10.1016/j.jaad.2020.04.049
- Firoz, B., Kovich, O. I., & Latkowski, J. A. (2007). Mycosis fungoides with depigmentation secondary to treatment. Dermatology online journal, 13(1), 18.

Cutis Journal
Read published peer-reviewed articles written your by Skin of Color Society members

Did You Know
Skin of color patients comprise the majority in California, New Mexico and Texas…and soon will be the majority in Arizona, Nevada, Georgia, New York and Florida.
By 2042, more than 50% of the US population will have skin of color.




